In clinical practice, we often view the skin and eyes as a “window” into the body’s internal chemistry. When a patient walks into my clinic with scleral icterus (yellowing of the white part of the eye), my mind immediately begins a differential diagnosis centered on the hepatobiliary system.
As health professionals, understanding the “why” behind this yellow pigment is crucial for moving from a simple observation to a definitive treatment plan.
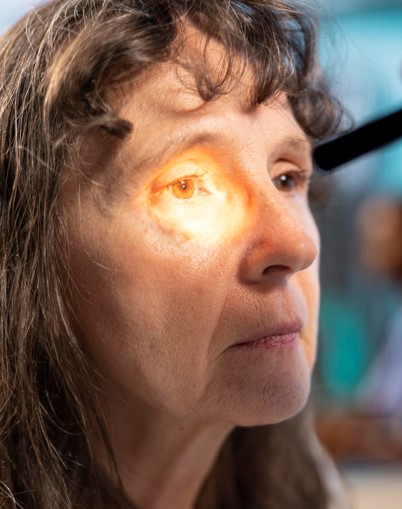
The Clinical Significance of the Sclera
Why do we look at the eyes first? The sclera contains high amounts of elastin, a protein that has a very high affinity for bilirubin. Jaundice typically becomes clinically visible in the eyes when serum bilirubin levels exceed 2.5 to 3.0 mg/dL. This is often the first physical sign of liver stress, appearing well before the skin turns yellow.
The Pathophysiology: The Bilirubin “Logjam”
Bilirubin is the byproduct of hemoglobin breakdown. Think of the liver as a processing plant that must “package” (conjugate) this bilirubin to make it water-soluble so it can be excreted.
When you see jaundice, that processing plant is failing for one of three reasons:
- Pre-hepatic: Too much “raw material” (excessive breakdown of red blood cells/hemolysis).
- Intra-hepatic: The “plant” is damaged (Hepatitis, Cirrhosis, or drug-induced injury).
- Post-hepatic: The “delivery trucks” are blocked (Gallstones or tumors obstructing the bile duct).
Interpreting the Liver Function Test (LFT) Panel
When I order an LFT panel in response to jaundice, I am looking for specific patterns to determine the source of the injury:
| Lab Marker | Physician’s Interpretation |
| ALT (Alanine Aminotransferase) | The most specific marker for hepatocellular injury (liver cell death). |
| AST (Aspartate Aminotransferase) | Also indicates liver damage, but can also be found in heart and muscle tissue. |
| ALP (Alkaline Phosphatase) | If significantly elevated compared to ALT/AST, I suspect a bile duct obstruction. |
| Bilirubin (Direct vs. Indirect) | Tells me if the problem is in the processing (Indirect) or the excretion (Direct). |
The Doctor’s “Next Steps”
If a patient presents with jaundiced sclera and elevated LFTs, our diagnostic journey usually follows this path:
- Imaging: An abdominal ultrasound or CT scan to check for physical blockages (stones or masses).
- Serology: Testing for viral hepatitis (A, B, or C) or autoimmune markers.
- Medication Review: Ruling out drug-induced liver injury (DILI)—even common over-the-counter meds like acetaminophen can be the culprit.
A Message for the Care Team
For the nursing and clinical staff, your role in monitoring these patients is vital. Beyond the labs, watch for mental status changes (hepatic encephalopathy) or increased bruising (coagulopathy). These clinical signs, paired with the LFT trends, tell us how the patient is truly responding to our intervention.
