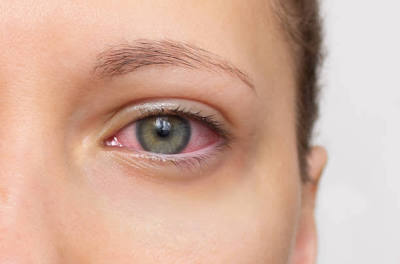
Uveitis is a serious eye condition characterized by inflammation of the uvea, the middle layer of the eye responsible for supplying blood to the retina. This condition can affect one or both eyes and, if left untreated, may lead to vision loss or other complications. Understanding its causes, symptoms, and proper nursing care is essential for effective management and prevention of long-term damage.
What Is the Uvea?
The uvea is the middle layer of the eye that lies between the sclera (the white outer layer) and the retina (the inner light-sensitive layer). It consists of three main parts:
- Iris – the colored part of the eye that controls pupil size.
- Ciliary body – responsible for producing aqueous humor and controlling lens shape.
- Choroid – a layer rich in blood vessels that nourish the retina.
When any of these structures become inflamed, the condition is collectively referred to as uveitis.
Types of Uveitis
Uveitis is classified based on the part of the uvea that is affected:
- Anterior Uveitis (Iritis) – affects the iris; the most common and usually less severe.
- Intermediate Uveitis – involves the ciliary body.
- Posterior Uveitis – affects the choroid and retina; may cause significant vision problems.
- Panuveitis – inflammation of all parts of the uvea.
Causes and Mechanism
Uveitis can occur due to a variety of causes. The inflammation may result from:
- Infections: such as herpes, tuberculosis, or syphilis.
- Autoimmune disorders: like rheumatoid arthritis, lupus, or sarcoidosis, where the immune system mistakenly attacks the body’s own tissues.
- Trauma: injury to the eye can trigger an inflammatory response.
- Unknown causes (Idiopathic): in some cases, the exact cause cannot be identified.
The mechanism involves the immune system’s reaction to a perceived threat, causing inflammation of the uvea. This inflammation leads to swelling, pain, and possible damage to surrounding eye tissues.
Signs and Symptoms
Common symptoms of uveitis include:
- Eye redness
- Eye pain or discomfort
- Blurred or decreased vision
- Sensitivity to light (photophobia)
- Floaters (dark spots in vision)
If these symptoms appear suddenly, it is crucial to seek immediate medical attention from an ophthalmologist.

Diagnosis
Diagnosis of uveitis involves a comprehensive eye examination, which may include:
- Slit-lamp examination to check for inflammation.
- Eye pressure measurement (tonometry).
- Blood tests or imaging to identify any underlying infection or autoimmune condition.
Prompt diagnosis is essential for preventing complications such as glaucoma, cataract, or retinal damage.
Treatment
The treatment approach depends on the cause and severity of the inflammation. It typically includes:
- Corticosteroid eye drops or injections to reduce inflammation.
- Antibiotics or antivirals if infection is present.
- Immunosuppressive drugs for autoimmune-related cases.
- Pain relief and pupil-dilating drops to reduce discomfort and prevent scarring.
Regular follow-up with an eye specialist is critical to monitor response and adjust therapy as needed.
Nursing Care and Management
Nursing care plays a vital role in supporting patients with uveitis. Key responsibilities include:
- Coordinating care with ophthalmologists and other specialists to ensure effective treatment.
- Managing pain through prescribed medications and patient comfort measures.
- Educating the patient about the importance of:
- Adhering to medication schedules.
- Attending regular follow-up appointments.
- Protecting the eyes from bright light and trauma.
Nurses also monitor for side effects of corticosteroids and help patients recognize early signs of recurrence.
Prevention and Long-Term Outlook
While not all cases of uveitis are preventable, maintaining good overall health and managing autoimmune or infectious diseases can reduce risk. With early detection and proper treatment, most patients recover well without permanent vision loss.
Uveitis is an inflammatory eye disorder that requires timely diagnosis, appropriate medical management, and coordinated nursing care. Understanding its causes, symptoms, and treatment options empowers patients to take better care of their eye health. Collaboration between healthcare professionals and patients is essential to prevent complications and preserve vision.